Capnography
What is Capnography?
The lungs have two main functions: to inhale oxygen (O2) into the body and to exhale carbon dioxide (CO2) from the body. In normal lungs, the amount of CO2 exhaled is very close to the level of carbon dioxide in the blood.
Capnography indicates how much CO2 is being eliminated from the lungs by measuring exhaled CO2 with a device that senses the CO2 level. It is a sensitive indicator of lung function and may help guide the doctor, nurse, or respiratory therapist to adjust the breathing machine or it may provide an early warning that the lungs are not functioning properly.
Capnography is also widely used as a safety device because it is a fast and reliable indicator of proper placement of a breathing (endotracheal) tube, which is a tube extending from the nose or mouth into the windpipe. Not all ICU patients require capnography.
What is a capnography monitor?
Capnography is accomplished by the attachment of a CO2 detection device to both the breathing tube and the capnography monitor. The CO2 detection device measures the level of exhaled CO2 in the breathing tube and transmits that information to the capnography monitor, which displays the exhaled CO2 level. When the amount of CO2 coming from the lungs is abnormally high or low, the capnography monitor alerts the ICU staff of a potential problem with the patient and prompts further investigation. Also, if the breathing tube becomes dislodged or disconnected, the capnography monitor alerts the ICU staff. The monitor helps the ICU staff monitor lung function without drawing blood so often.
How long is capnography used?
Capnography is used as long as the ICU staff feels that it provides benefit for the patient.
What is a normal reading?
Normal levels vary between 30-40. An alarm alerts the nurses if the reading gets too low or too high.
Does capnography hurt?
The device is harmless and causes no pain.
Are there any potential complications associated with capnography?
There are no significant complications associated with capnography.
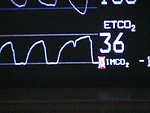
Capnography waveform (ETCO2 - 36) displayed on a bedside monitor
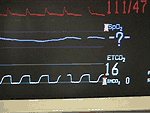
Capnography (ETCO2 - 16) indicating a lower than normal value, displayed on a bedside monitor